What have we learnt from the coronavirus outlier?
We now know much more about Covid-19 than we did even a month ago.
First, serology tests have shown that only fairly small numbers of people in Europe and the US have had Covid-19 (and nearly everyone who has had the virus seems to get antibodies against it).
In the UK, a study reported by the Health Secretary indicated that about 5% of the population nationwide has had it, and about 17% of Londoners. A large serology study in Spain found antibodies in around 5% of the population, a study in Milan found antibodies in 4.4-10.8% of the population, and a recent Bayesian estimation of the IFR for US states using data from European countries found about 4% nationwide prevalence, and around 16.6% prevalence in New York.
Second, the number of deaths combined with those antibody test results are consistent with an infection fatality rate (IFR) in the order of 0.49-1.01%. This may be a conservative estimate, since not all deaths caused by Covid have been confirmed as such (for example, in the UK’s care homes, which have had a hugely elevated death rate during the past few months).
Third, Covid-19 appears to kill people who still have a long life ahead of them. One study suggests that on average, men who die of Covid would have had another 13 years to live, and women another 11 years to live. These figures are already adjusted for comorbidities that would shorten their lives.
Attempts to downplay the severity of Covid-19 usually ignore or obfuscate one or more of the above factors. Some, even from experts, are just innumerate. The disease simply cannot have an infection fatality rate of one in ten thousand with at least 36,000 deaths in a population of 66 million, for example, despite the claims of one Oxford epidemiologist.
All of these appear to weigh in favour of the lockdown having been the correct course of action, and against a rapid end to the lockdown — until we have appropriate measures in place to ensure we do not get a second uncontrollable outbreak of the disease.
However, a fourth fact seems to stand against this: the Swedish experience. Sweden did not impose as strict a lockdown as most developed countries, but it still avoided the sort of death rates that many (including the authors of this piece) had feared.
But while Sweden may suggest that the benefits of lockdown have been overstated, it also shows that the costs have too. And there are good reasons to think that Sweden has had many of the costs of mandatory lockdowns, with few of the benefits.
Voluntary distancing without a lockdown
Applied to Sweden by researchers at Uppsala University, the Imperial College model that guided the UK’s policy decisions suggested that up to 40,000 would die from coronavirus by the end of April if no mitigations had been put in place. Alternatively, a naïve application of an IFR of 0.75% and a herd immunity threshold of 60% (based on a reproduction rate of 2.5 per case) puts that figure at 45,000. And yet, at the time of writing, Sweden’s death toll is just below 4,000.
While Sweden did not impose anywhere near as restrictive a set of measures as its neighbours Norway and Denmark, per capita deaths attributed to Covid-19 are four times higher than in Denmark and nine times higher than in Norway and Finland. (Because of potentially unobservable differences in countries, such as culture or climate, we try to compare Sweden with its neighbours throughout.)
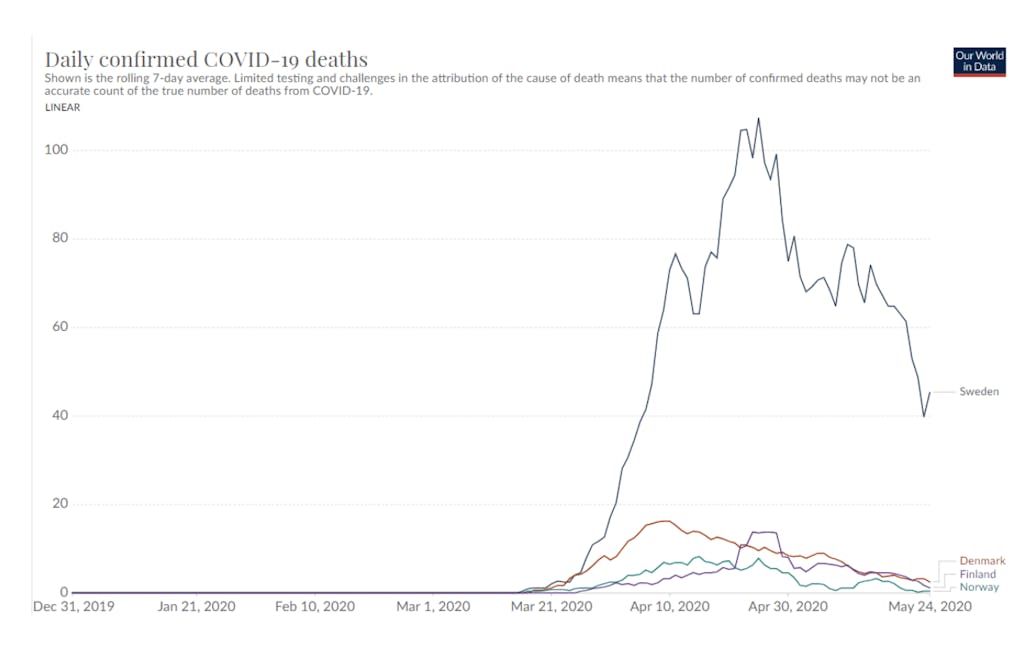
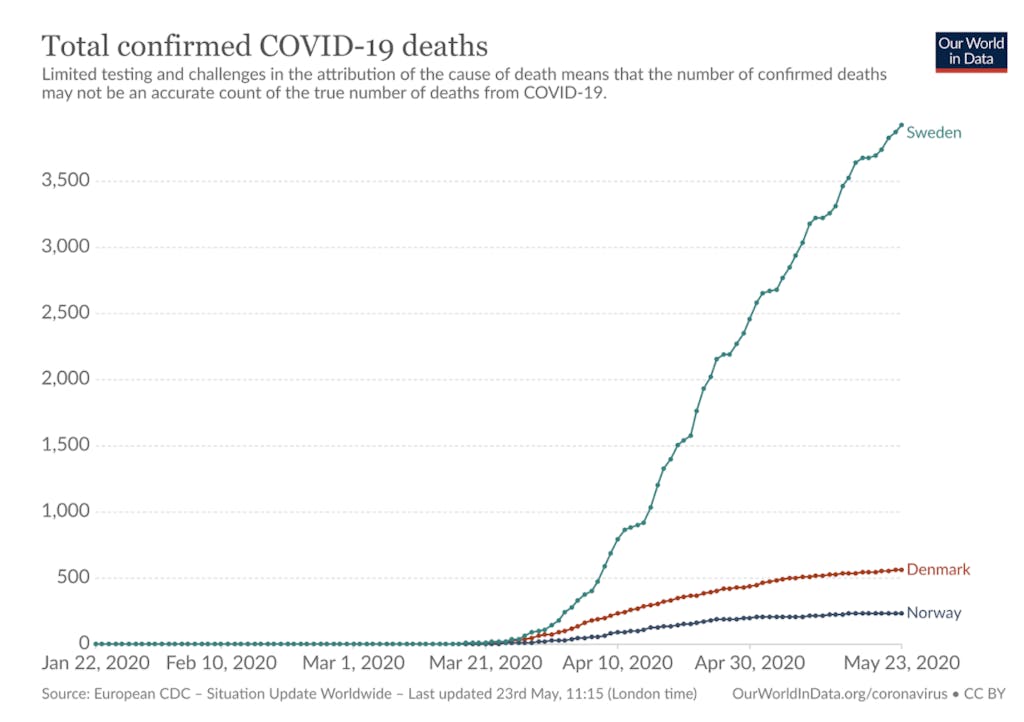 Sweden has also, at the time of writing, only just reached a point where daily deaths have started falling, if it has at all — a point which Denmark and Norway reached in early April. (Readers have pointed out while deaths peaked in mid-April, and decreased from an earlier plateau of around 80 per day, modelling suggests that daily deaths are currently at an estimated value of around 60 per day. Note that Sweden’s per day fatality counts are initially undercounted and revised upwards later due to reporting delays, which models such as this attempt to account for.)
Sweden has also, at the time of writing, only just reached a point where daily deaths have started falling, if it has at all — a point which Denmark and Norway reached in early April. (Readers have pointed out while deaths peaked in mid-April, and decreased from an earlier plateau of around 80 per day, modelling suggests that daily deaths are currently at an estimated value of around 60 per day. Note that Sweden’s per day fatality counts are initially undercounted and revised upwards later due to reporting delays, which models such as this attempt to account for.)
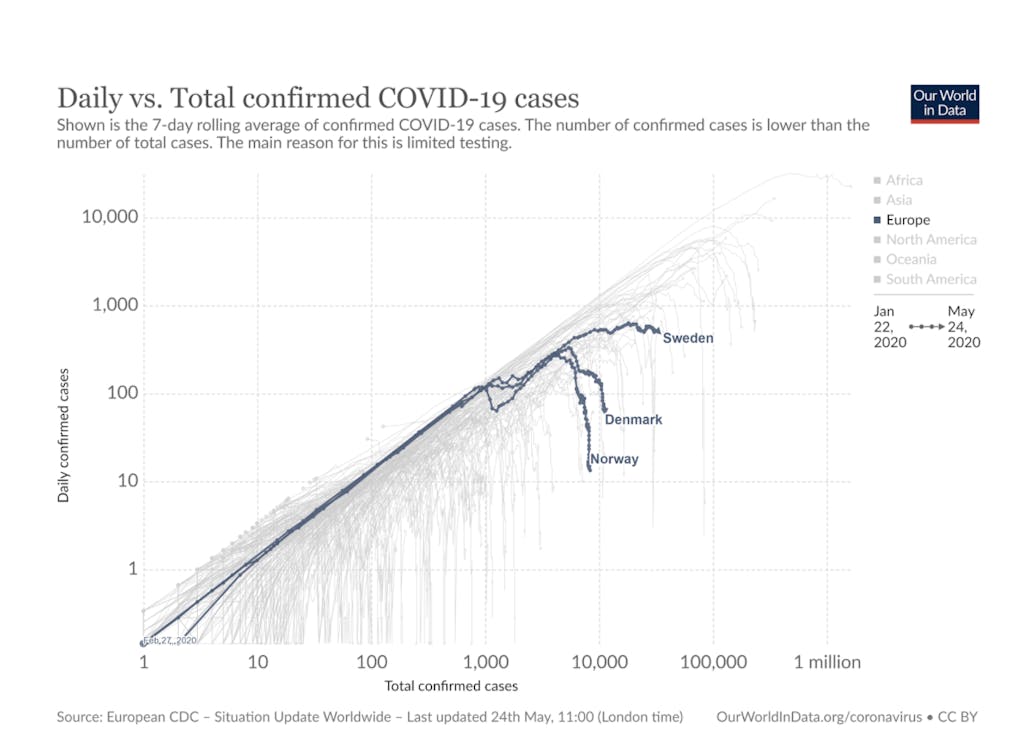
 Similarly, the number of cases in Sweden has not yet started falling, suggesting that Sweden’s outbreak has further to go, and more people to kill. (We use case numbers with some caution, because its current fatality rate per confirmed case is 12%, suggesting that Sweden is significantly undercounting cases.)
Similarly, the number of cases in Sweden has not yet started falling, suggesting that Sweden’s outbreak has further to go, and more people to kill. (We use case numbers with some caution, because its current fatality rate per confirmed case is 12%, suggesting that Sweden is significantly undercounting cases.)
 It is a mistake to imagine that Sweden had no lockdown at all. The Swedish government recommended that over-70s stop spending time with others, that people work from home where possible, and that large gatherings not be held — but, as Johan Norberg writes, the Swedish police do not have the power to break up large gatherings if they do come together. Sweden also closed universities and high schools.
It is a mistake to imagine that Sweden had no lockdown at all. The Swedish government recommended that over-70s stop spending time with others, that people work from home where possible, and that large gatherings not be held — but, as Johan Norberg writes, the Swedish police do not have the power to break up large gatherings if they do come together. Sweden also closed universities and high schools.
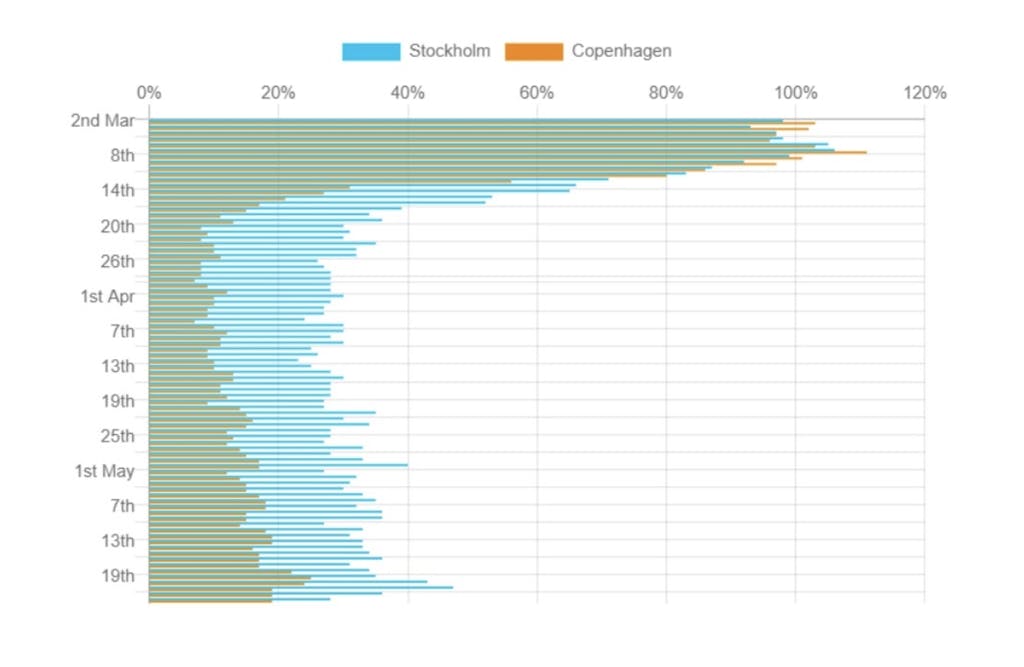
But, even without a mandatory lockdown that kept people in their homes and closed businesses, many Swedes engaged in voluntary, individual distancing. For example, Swedes are travelling much less now than in normal times. The Citymapper mobility index, compiled by a popular journey-planning app, compares the percentage of users planning trips using the app compared to normal. A comparison of Copenhagen and Stockholm, the epicentres of the epidemic in Denmark and Sweden, suggests a very pronounced reduction in travel starting roughly on the 13th of March in both cities: down to around 10-15% of normal in Copenhagen, and around 30-35% in Stockholm.
 Retail activity has fallen by just over 40% in the two largest counties in the country, while Stockholm’s public transport company reports a 50% decrease in the number of passengers on the underground and on commuter trains. There is also survey evidence suggesting around half of the labour force in Stockholm is working remotely. Additionally, the government has imposed some measures restricting large gatherings and shutting down establishments that do not adhere to social distancing norms.
Retail activity has fallen by just over 40% in the two largest counties in the country, while Stockholm’s public transport company reports a 50% decrease in the number of passengers on the underground and on commuter trains. There is also survey evidence suggesting around half of the labour force in Stockholm is working remotely. Additionally, the government has imposed some measures restricting large gatherings and shutting down establishments that do not adhere to social distancing norms.
Did Sweden get it right?
All of this suggests that the degree of distancing that people will voluntarily do has turned out to be far greater than most analysts realised.
And with this large degree of voluntary distancing, Sweden has not done nearly as badly as many had feared. Does this mean Sweden has done well? Is Sweden a model that other countries could have followed, or could follow now by ending its own lockdowns suddenly?
Probably not. Sweden has fallen between two stools: because of voluntary social distancing, it has not achieved herd immunity, or anything like it, but it also has not suppressed the virus as countries that have had a lockdown have. According to a recent study by Sweden’s public health agency, only 7.3% of the population of Stockholm has Covid-19 antibodies (compared to a reported 17% of Londoners, for example), and only 15% at a Stockholm hospital (which can act as an upper bound, since healthcare workers are most likely to be exposed to the virus).
Sweden has also not been able to shield older people. Care home residents account for nearly half of Sweden’s Covid-19 deaths. So any hope that the country could allow younger people to catch it and keep older people safe seems dashed.
Since we now know the disease’s IFR is somewhere around 0.5-1%, it is hard to see how Sweden could achieve herd immunity without reaching the scale of deaths that people initially feared it would get without a lockdown. Sweden’s death rate so far is consistent with around 7% or less of the population having had the virus and an IFR of 0.5% or higher.
Did Sweden avoid the economic contractions that countries with stricter lockdowns have suffered? So far, it appears not. The European Commission forecasts a reduction in Swedish GDP of 6.1% for 2020, which is comparable to a projected fall of 5.5% and 5.9% in the GDP of its neighbours Norway and Denmark respectively. Like most Scandinavian countries, Sweden is a small open economy that is very exposed to foreign trade shocks, but the EC’s forecast is driven by sharp falls in domestic consumption and investment as well as foreign trade shocks. As Ryan Bourne has argued, “Just because people are free to engage in economic activities or open their businesses, does not mean workers or businesses will do so.”
A final reason to worry about Sweden’s as-yet uncontrolled outbreak is that it makes it difficult for the country to change course and opt for the sort of contact tracing and case isolation strategy that some Asian countries have used with some success, and which many Western countries are now attempting. Contact tracing programmes may not be feasible without a low initial base of cases, according to this discussion of the evidence, and getting there may require Sweden to opt for a strict lockdown even after its neighbours have ended theirs.
It is also worth stressing that Sweden is probably not much better prepared for another wave of the virus, because so few Swedes have been infected. (However, this may be wrong if it turns out that some people spread the disease more than others, and that these people have already been infected in places like Sweden and the UK but not in places that had smaller outbreaks.)
Live free and die
Clearly the Swedish approach does have some benefits. Swedes are freer to enjoy their lives without the constraints imposed by governments of other countries, and much of this is unlikely to be captured in official GDP statistics. There are huge costs to preventing people from doing what they want to do, and it is virtually certain that lockdowns in other countries have banned activities that will turn out to have been fairly harmless.
Voluntary distancing also means that individuals can make judgements about costs and benefits that governments cannot. This could mean that Swedes could more easily prioritise activities that they value, but that governments do not.
The downside of this is that they will not always factor in the costs that these activities impose on others, such as people who may be mildly ill going to public places as normal and infecting many others.
Even with this additional degree of freedom, the severe limits to social life imposed by the virus itself are inescapable. Voluntarily choosing not to see your friends and family because you don’t want to kill them is not much better than being forced not to by the state.
Ultimately, Sweden shows that some of the worst fears about uncontrolled spread may have been overblown, because people will act themselves to stop it. But, equally, it shows that criticisms of lockdowns tend to ignore that the real counterfactual would not be business as usual, nor a rapid attainment of herd immunity, but a slow, brutal, and uncontrolled spread of the disease throughout the population, killing many people. Judging from serological data and deaths so far, it is the speed of deaths that people who warned in favour of lockdowns got wrong, not the scale.
The biggest cost of Sweden’s choice may be if other Western countries do successfully implement contact tracing-type strategies to suppress the virus until a permanent solution is found – as most countries do currently with any of the other deadly, contagious diseases that are not vaccinated against. If that happens, Sweden may be in the unenviable position of having too many cases to follow suit, without bringing in a lockdown of the kind that other countries did long before.
This is the challenge the UK government currently faces. Any attempt to bring an end to lockdown measures too soon may make contact tracing unviable because of the high number of daily new cases — a worry shared by some officials, according to an article in The Times.
While Sweden’s approach has clearly been more liberal than that of many other countries, it has also led to an uncontrolled outbreak that has killed many more people than in its neighbours. Depending on what comes next, it may prove to have been a colossal and deadly mistake.
Update: Since the time of writing, more recent modelling by Sweden’s Public Health Agency has estimated that “a little more than 20%” of Stockholm’s population is immune from the virus, putting it slightly ahead of the most recent London study.
